The delivery of modern medicine requires precision, speed, and seamless collaboration. Yet, unified clinical communication challenges continue to undermine clinical operations, creating a chaotic environment where vital patient data is scattered across incompatible channels.
We define unified clinical communication as the centralized, secure, and synchronized exchange of patient information, alerts, and care coordination protocols among healthcare professionals.
Unfortunately, what most healthcare organization and practices currently experience is fragmented healthcare communication, a disjointed web of legacy pagers, unencrypted text messages, EHR portals, and standalone messaging applications.
This fragmentation does not merely inconvenience staff; it actively threatens patient safety, escalates compliance risks, and drives profound inefficiency across care teams. As doctors and nurses are forced to navigate multiple screens to coordinate a single care episode, the administrative burden skyrockets.
The resulting friction directly fuels the ongoing crisis of physician burnout, stripping clinicians of the autonomy and time needed for direct patient care.
By addressing these unified clinical communication challenges head-on, medical leaders can transition from reactive, siloed workflows to proactive, intelligent, and highly optimized healthcare delivery.
Key Takeaways
| Challenge | Operational Impact | Compliance Risk | Strategic Solution |
|---|---|---|---|
| Fragmented communication tools | Delayed decision-making and workflow disruption | Inconsistent documentation | Unified clinical communication platform |
| Shadow IT usage | Data silos across personal devices | HIPAA violations and PHI exposure | HIPAA compliant clinical communication software |
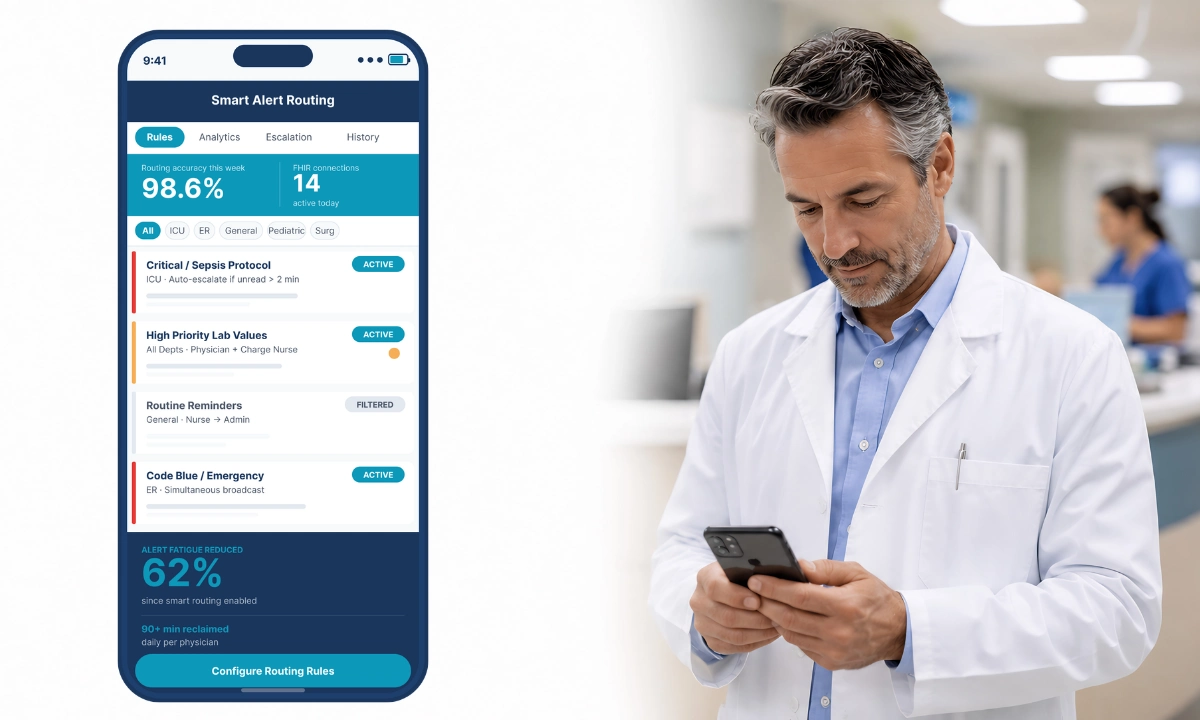
| Manual message routing | Lost physician time and burnout | Missed critical alerts | AI-powered smart routing |
| Undocumented consults | Revenue leakage and billing gaps | Incomplete audit trails | Secure, case-based collaboration |
| EHR inbox overload | Increased average length of stay (ALOS) | Delayed patient discharge | Centralized clinical messaging infrastructure |
What Are Unified Clinical Communication Challenges?
Unified clinical communication challenges are systemic operational barriers; such as alert fatigue, EHR integration gaps, and non-compliant messaging; that prevent healthcare teams from securely and efficiently sharing real-time patient data.
These breakdowns create workflow friction, delay clinical decision-making, and significantly increase the risk of physician burnout and HIPAA violations.
The core challenges disrupting modern medical operations include:
- Disjointed and fragmented healthcare communication platforms
- Severe alert fatigue from untargeted notifications
- The absence of real-time, role-based message routing
- Complex EHR integration challenges and data silos
- Shadow IT leading to severe HIPAA compliance risks
- Cognitive overload from constant application and tool switching
- Failure to leverage intelligent healthcare communication software and AI
The 7 Biggest Unified Clinical Communication Challenges
1. Fragmented Communication Systems
The foundation of modern clinical care requires a synchronized care team, yet fragmented communication systems force providers to piece together patient narratives from disparate sources.
A single patient transfer might involve a secure message, a phone call, an EHR inbox alert, and a paper sticky note. This disjointed ecosystem forces physicians to waste precious time hunting down colleagues or piecing together clinical context rather than delivering care.
The operational impact is severe: delayed handoffs, misaligned care plans, and increased length of stay. From an efficiency standpoint, navigating this fragmented healthcare communication landscape drains hours from the clinical week.
For the physician, this constant friction accelerates burnout, as the cognitive load of managing disjointed systems overshadows the practice of medicine.
Furthermore, this fragmentation drives care teams to bypass secure channels, directly increasing the risk of HIPAA violations and institutional liability.
Without a connected healthcare organization infrastructure layer, departments remain siloed and workflows break down across care settings.
2. Alert Fatigue and Notification Overload
Alert fatigue in healthcare is a critical patient safety and physician wellness issue.
When clinical communication software bombards providers with non-differentiated, low-priority notifications alongside critical alarms, the psychological response is desensitization.
Physicians and nurses are routinely subjected to hundreds of alerts per shift, the vast majority of which require no immediate clinical intervention.
The efficiency impact is profound, as constant interruptions derail deep clinical thinking and disrupt complex procedural workflows. Operationally, true emergencies can be missed in the noise of meaningless digital chatter.
The burnout impact is equally severe; the incessant cognitive interruption of notification overload drives profound emotional exhaustion and frustration.
Without a unified clinical communication platform capable of intelligent filtering, health systems inadvertently condition their most valuable assets to ignore the very systems designed to keep patients safe, escalating both clinical and compliance risks.
3. Lack of Real-Time Role-Based Routing
Healthcare is a dynamic, shift-based environment, yet many legacy communication systems rely on static directories.
The lack of real-time, role-based routing forces clinicians to manually cross-reference on-call schedules, whiteboards, and outdated phone trees to find the right specialist.
This unified clinical communication challenge causes immediate operational bottlenecks. If an attending physician needs a stat cardiology consult, sending a message to a named cardiologist who just went off shift delays life-saving interventions.
Efficiency plummets as nurses and doctors spend unbillable hours acting as switchboard operators. This manual routing exacerbates physician burnout by introducing unnecessary administrative friction into urgent clinical scenarios.
Furthermore, when messages are routed to the wrong provider, it creates a trail of undocumented, misdirected protected health information (PHI), exposing the medical practice to regulatory scrutiny and compliance failures.
4. EHR Integration Gaps
While Electronic Health Records (EHRs) are the legal source of truth, they are notoriously poor tools for real-time collaboration.
EHR integration challenges occur when communication platforms operate outside the patient’s chart, stripping messages of vital clinical context.
A secure text saying “Please review room 402” requires the receiving physician to independently log into the EHR, locate the patient, and hunt for recent labs or vital changes.
This lack of interoperability cripples medical practice efficiency. Operationally, it slows down discharge planning, medication approvals, and cross-specialty consults.
The burnout impact is direct: physicians deeply resent the “clicks” required to toggle between communication silos and the EHR.
When clinical workflow optimization is blocked by these integration gaps, clinicians often resort to verbal orders or undocumented curbside consults, risking data integrity and creating compliance gaps in the legal medical record.
5. Shadow IT and HIPAA Risk
When official healthcare communication software is cumbersome, slow, or poorly designed, clinicians will inevitably find their own workarounds. This phenomenon, known as Shadow IT, typically manifests as care teams using consumer-grade messaging apps (like iMessage or WhatsApp) to coordinate care.
The operational impact is a completely fractured communication landscape where critical patient data lives on personal, unencrypted devices.
True HIPAA compliant collaboration requires purpose-built hipaa compliant clinical communication software that delivers encrypted messaging, secure voice, and case-based discussions inside a protected ecosystem.
Efficiency might seemingly improve for the individual user, but institutional efficiency collapses because these conversations are siloed and inaccessible to the broader care team.
The compliance risk is catastrophic: transmitting PHI over consumer networks is a direct violation of federal law, inviting massive fines and institutional reputational damage.
While this workaround temporarily reduces the friction that causes physician burnout, it replaces it with the profound legal anxiety of operating outside of HIPAA compliant collaboration frameworks.
6. Workflow Disruption from Tool Switching
Modern physicians do not just suffer from too many patients; they suffer from too many screens.
Workflow disruption from tool switching occurs when a clinician must use a pager for codes, a secure texting app for consults, an EHR portal for patient messages, and a separate application for viewing on-call schedules.
This constant context switching destroys clinical workflow optimization. The operational impact is a highly inefficient care delivery model characterized by start-and-stop momentum.
Efficiency is lost in the micro-seconds and minutes spent logging in, authenticating, and navigating different user interfaces. The burnout impact is insidious; it creates a relentless, underlying cognitive burden that leaves physicians exhausted at the end of a shift, feeling like data-entry clerks rather than healers.
Consolidating these tools into a single, cohesive unified clinical communication platform is essential for restoring clinician focus.
7. Underutilized AI in Clinical Communication
Despite massive advancements in artificial intelligence, clinical communication remains largely stuck in the era of basic, rules-based text routing. The underutilization of healthcare AI communication represents a massive missed opportunity for health systems.
Operationally, without AI to triage, summarize, and prioritize inbound messages, the burden of determining urgency falls entirely on the receiving physician.
The efficiency impact is a systemic failure to scale; human providers cannot manually process the exponential growth of clinical data points and messages without AI augmentation.
This lack of intelligent support accelerates burnout, as clinicians are left to manage the data deluge unaided. From a compliance perspective, advanced AI can monitor communication networks for policy violations and secure data routing, a capability entirely lost when health systems rely on legacy communication infrastructure.
How These Challenges Impact Medical Practice Efficiency
The cascading effects of unified clinical communication challenges directly erode the financial and operational foundation of healthcare organizations. Poor communication architecture actively blocks clinical workflow optimization, transforming highly trained specialists into administrative coordinators.
First, the time loss per physician is staggering. Industry data suggests that clinicians can lose up to 45 to 50 minutes to an hour every shift simply attempting to locate colleagues, verify on-call schedules, or clarify poorly routed messages. This is not merely an inconvenience; it represents a massive bottleneck in patient throughput.
Delayed decision-making follows closely. When a critical lab result sits unread in an EHR inbox because it wasn’t pushed through a secure clinical messaging system, patient discharge is delayed. This increases the average length of stay (ALOS), directly impacting hospital capacity and medical practice efficiency.
Furthermore, fragmented communication leads to significant revenue leakage from undocumented consults. When physicians engage in quick, unrecorded “curbside consults” in the hallway or via consumer text messaging, the time spent delivering that expertise cannot be properly coded or billed.
The administrative burden of manually transcribing these interactions back into the official record is often ignored, resulting in lost revenue.
A robust unified clinical communication platform captures these interactions within the secure ecosystem, ensuring that all clinical effort is documented, compliant, and appropriately valued.
The Hidden Link Between Communication Failures and Physician Burnout
Physician burnout is rarely caused by the actual practice of medicine; it is driven by the systemic friction surrounding patient care.
Unified clinical communication challenges are a primary culprit in this crisis. When healthcare organizations fail to implement HIPAA compliant collaboration tools that actually align with clinical realities, they systematically degrade the daily experience of their medical staff.
Alert fatigue is perhaps the most visible driver. The continuous buzzing of pagers and non-critical app notifications fragments a physician’s attention, preventing the deep focus required for complex diagnoses. This constant interruption breeds profound emotional exhaustion.
Poor communication architecture actively blocks clinical workflow optimization, undermining efforts focused on improving medical practice efficiency, and transforming highly trained specialists into administrative coordinators.
Physician isolation also grows when fragmented healthcare communication systems make it difficult to quickly consult with peers. Instead of a cohesive, supportive care team, providers feel like they are operating in silos.
Achieving true physician burnout reduction requires treating communication infrastructure not merely as an IT project, but as a core component of clinical well-being. By streamlining workflows and reducing administrative friction, health systems can return autonomy and time to their clinical teams.
How Healthcare AI and Innovation Can Solve These Challenges
The next generation of healthcare operations requires moving beyond static messaging apps into intelligent, dynamic ecosystems. Healthcare AI communication is uniquely positioned to solve the most intractable unified clinical communication challenges by serving as an invisible, highly efficient cognitive assistant for the care team.
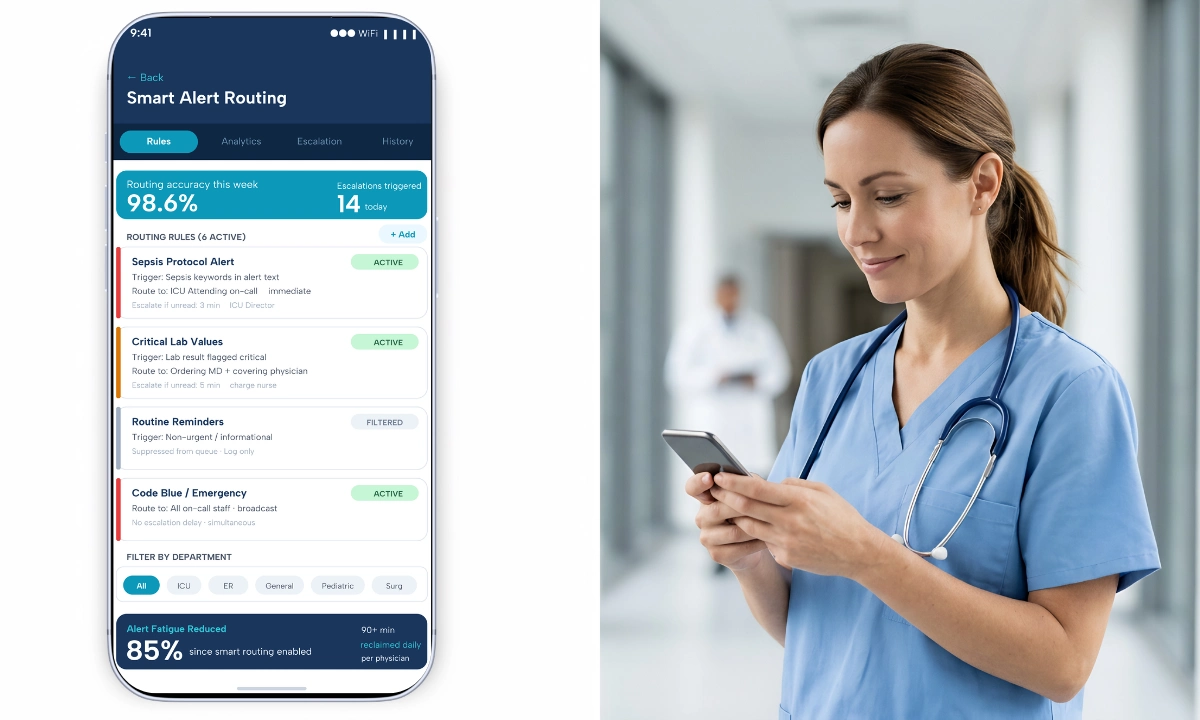
Smart routing and predictive prioritization are transforming how messages reach providers. Instead of relying on static directories, AI can instantly analyze the intent of a message, reference the live EHR context, check real-time location and shift data, and route the communication to the exact right physician.
To combat alert fatigue in healthcare, AI-powered alert reduction algorithms can ingest hundreds of telemetry alarms, filter out the clinical “noise” and transient artifacts, and only escalate genuinely actionable notifications to the clinician’s mobile device.
Advanced healthcare AI communication tools can triage and prioritize messages before they ever reach the physician.
Additionally, NLP-assisted documentation (Natural Language Processing) allows physicians to dictate consults and messages naturally, with the AI automatically structuring the data and pushing it directly into the EHR chart. Crucially, the deployment of Explainable AI ensures that when an algorithm prioritizes a message, the physician understands why.
Conclusion: The Future of Unified Clinical Communication
The era of tolerating disjointed, frustrating, and inefficient workflows in medicine must end. The urgency to address unified clinical communication challenges has never been greater, driven by an unsustainable physician burnout crisis, stringent compliance mandates, and the absolute necessity for medical practice efficiency. Health systems can no longer afford the revenue leakage, delayed patient care, and staff turnover associated with fragmented healthcare communication.
The transition to a unified clinical communication platform represents a massive operational opportunity. By bridging EHR integration gaps, eliminating shadow IT, and embracing intelligent healthcare AI communication, organizations can fundamentally transform how care is delivered.
It is an innovation advantage that protects institutional compliance while dramatically improving the daily lives of clinicians.
Solving these challenges is not simply an upgrade in technology; it is a commitment to the people who deliver care.
We invite medical leaders, hospital executives, and practice managers to secure early access and explore how an intelligent, physician-designed communication ecosystem can restore the joy of practicing medicine, streamline your operations, and safeguard your patients.
Summary
Unified clinical communication challenges stem from fragmented messaging systems, EHR integration gaps, alert fatigue, and non-compliant communication practices. These breakdowns increase physician burnout, delay decision-making, and reduce medical practice efficiency. AI-powered, HIPAA-compliant unified clinical communication platforms solve these issues through intelligent routing, alert filtering, secure messaging, and real-time EHR integration.
This improves workflow optimization, protects PHI, and restores clinician focus.
Frequently Asked Questions
What is unified clinical communication?
Unified clinical communication is an integrated technology framework that consolidates voice, text, alerts, and on-call scheduling into a single, secure platform. It connects seamlessly with the Electronic Health Record (EHR) to ensure that the entire care team can collaborate in real-time, sharing patient data efficiently without switching between disjointed applications or legacy pagers.
Why is fragmented communication dangerous in healthcare?
Fragmented healthcare communication forces providers to use multiple, disconnected tools to share critical patient data. This disjointed approach leads to delayed clinical decisions, misdirected messages, and lost test results. It compromises patient safety, extends hospital length of stay, and drives severe inefficiencies that disrupt overall medical practice operations.
How does poor communication increase physician burnout?
Poor communication systems cause constant interruptions, severe alert fatigue, and high administrative burden. When physicians waste hours navigating clunky software, hunting down colleagues, or fielding off-duty messages due to bad routing, it causes emotional exhaustion. Effective clinical workflow optimization directly contributes to meaningful physician burnout reduction by restoring clinical autonomy.
What makes a communication platform HIPAA compliant?
HIPAA compliant collaboration requires end-to-end encryption for all protected health information (PHI) both in transit and at rest. It must include strict access controls, secure user authentication, remote wipe capabilities for lost devices, and comprehensive audit logs that track exactly who accessed or transmitted specific patient data and when.
How can AI improve clinical collaboration?
Healthcare AI communication improves collaboration by acting as an intelligent triage system. AI can drastically reduce alert fatigue by filtering non-actionable alarms, predictively route messages to the correct on-call specialist based on real-time data, and use natural language processing to assist with seamless documentation, thereby optimizing overall medical practice efficiency.