Multi-Modal Clinical Communication in Healthcare is transforming how medical teams coordinate care across increasingly complex environments. By integrating video, voice, and text within a governed infrastructure, healthcare organizations can reduce fragmentation, preserve context, and strengthen documentation integrity.
A unified clinical communication platform serves as the structural foundation that enables this convergence, ensuring audit-ready documentation and coordinated care delivery.
Summary
The modern medical landscape is currently navigating an unprecedented period of transition. As we move further into 2026, traditional healthcare communication methods are no longer sufficient to meet the demands of a complex, data-driven environment. Healthcare systems are currently burdened by a reliance on fragmented tools such as pagers, personal mobile devices, and unencrypted email, which has created what industry experts call a last-mile communication problem.
The economic and human toll is severe. Peer-reviewed research published in the National Library of Medicine estimates that communication inefficiencies alone cost U.S. hospitals more than $12 billion annually, with increased length of stay accounting for over half of that burden.
To resolve these structural deficits, forward-thinking medical organizations are pivoting toward a comprehensive strategy that integrates video, voice, and text into a single, secure ecosystem.
Implementing an integrated clinical communication infrastructure is no longer merely an IT upgrade; it is a fundamental requirement for maintaining operational viability, retaining clinical staff, and ensuring patient safety.
Key Takeaways for Healthcare Leaders
| Strategic Domain | Key Insight | Why It Matters |
|---|---|---|
| Communication Infrastructure | A governed clinical communication infrastructure integrates video, voice, and text within a secure environment. | Reduces modality fragmentation and preserves conversational context. |
| Financial Impact | Hospital communication inefficiencies cost U.S. hospitals over $12 billion annually. | Communication architecture directly affects operational margins and length of stay. |
| Burnout Reduction | Ambient documentation technology has been associated with significant reductions in clinician burnout (JAMA Network Open, 2025). | Reducing cognitive burden strengthens retention and well-being. |
| Revenue Integrity | CPT codes 99446–99452 require structured documentation for interprofessional consults. | Embedded documentation workflows improve audit readiness and reimbursement accuracy. |
| Governance & Compliance | HIPAA-aligned environments must distinguish PHI-enabled collaboration from non-clinical professional discussion spaces. | Clear governance boundaries reduce compliance risk. |
| Operational Efficiency | Unified communication reduces redundant messaging, rework, and context switching. | Improves response time and interdisciplinary coordination. |
Fragmented clinical communication creates measurable enterprise risk. Inefficiencies increase length of stay, accelerate physician burnout, elevate HIPAA exposure, and drive revenue leakage. When video, voice, and text operate in silos, coordination slows and audit gaps expand. Converged, governed communication infrastructure is now an operational and financial necessity.
What Is Multi-Modal Clinical Communication in Healthcare?
Multi-Modal Clinical Communication in Healthcare refers to the structured integration of video, voice, and text within a governed medical communication ecosystem.
At its core, an integrated clinical communication system represents a structural shift in how medical information is transmitted, stored, and utilized.
It replaces disparate, single-function tools with a cohesive system designed specifically for the rigors of healthcare. To address current clinical challenges, the industry must embrace a unified communication strategy that integrates video, voice, and text into a single, secure ecosystem.
This trinity of communication modalities represents the foundation of a resilient healthcare system.
By leveraging purpose-built, physician-centric unified clinical communication platform, medical practices can bridge the gaps that have historically plagued clinical workflows. These platforms are designed to unify video, voice, and text within a HIPAA-compliant governance framework.
Healthcare executives increasingly recognize that unified communication architecture is central to synchronizing clinical and administrative operations.
The Hidden Risk of Modality Fragmentation in Healthcare
The financial and human costs of inefficient communication are staggering. The reliance on fragmented tools such as pagers, personal mobile devices, and unencrypted email has created what industry experts call a last-mile communication problem. This failure to deliver the right information to the right person at the right time is more than a mere inconvenience.
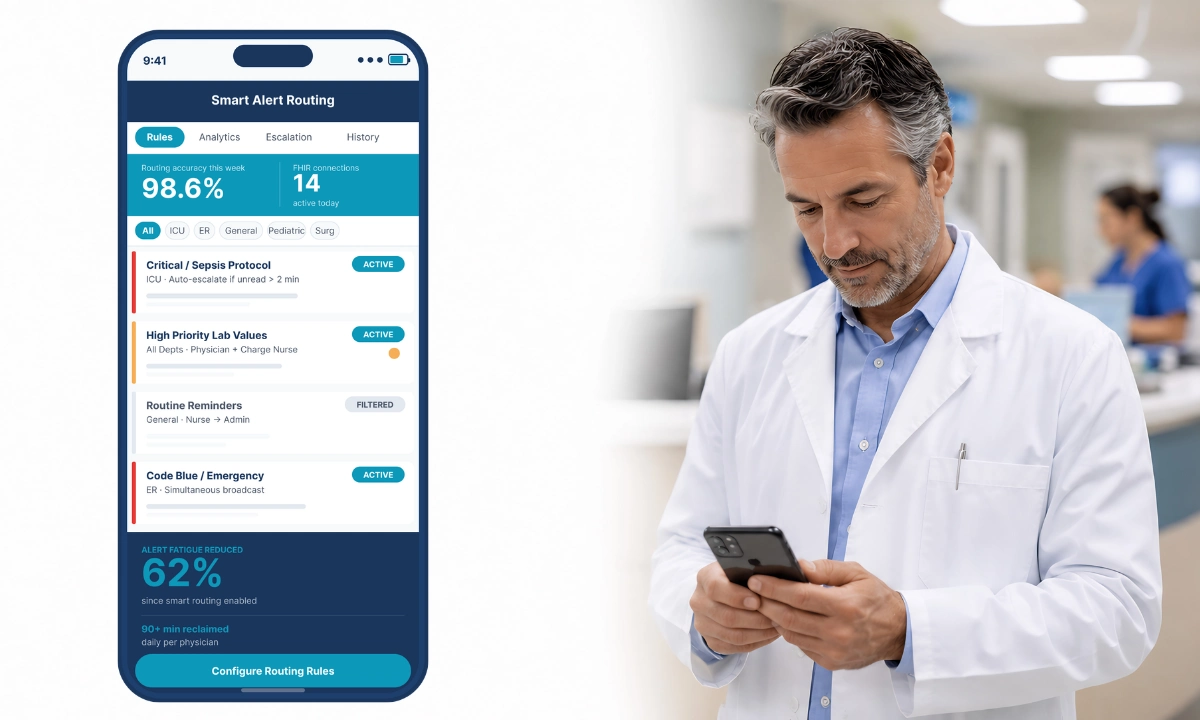
Recent data from the 2026 State of Nursing Communication Report indicates that while hospitals are communicating more frequently, they are not doing so effectively. Approximately 86 percent of hospitals still rely on email as their primary communication channel, despite nursing being a shift-based, deskless profession. This misalignment leads to a situation in which one-third of nurses report they do not have time to read updates during their shifts, and nearly half find the messages they receive to be only marginally relevant to their roles. Furthermore, 66% of nurses report skimming or deleting messages. This administrative friction ultimately serves as a primary driver of clinician burnout and a significant barrier to optimal patient outcomes.
These breakdowns mirror patterns documented in analyses of clinical communication failures in healthcare, where modality gaps often precede adverse events.
Why Video, Voice, and Text Must Function as One System
An integrated clinical communication ecosystem must offer distinct, yet connected, modalities to capture the full spectrum of clinical interaction.
The Power of Video:
Linear and Non-linear Video communication has evolved beyond simple telehealth visits. Within a professional medical practice, video serves two primary functions:
- Linear Video: Real-time consultations and virtual huddles allow for face-to-face interaction, which is essential for reading non-verbal cues and building trust among team members.
- Non-Linear Video: Asynchronous video updates allow clinicians to share complex case details or shift handoff information that can be viewed at the receiving party’s convenience. This capability is central to intra-office unified communication modules that streamline department-level collaboration.
The Nuance of Voice: While text is efficient, voice remains the most effective way to convey urgency and nuance. Voice communication allows for immediate clarification and the expression of clinical intuition that might be lost in a written message. Integrating voice into a unified platform enables a provider to escalate a text conversation to a voice call with a single click, preserving the discussion’s context.
The Precision of Text: Text communication provides a structured, searchable record of interactions. Within inter-organizational collaboration modules, secure text messaging enables providers across hospitals and clinics to engage in dynamic consultations. These interactions can be embedded with documentation, capturing the reasoning and decision trails necessary for both clinical clarity and compliant revenue generation.
This convergence model represents the operational core of Multi-Modal Clinical Communication in Healthcare, where modality escalation preserves clinical nuance without sacrificing documentation integrity.
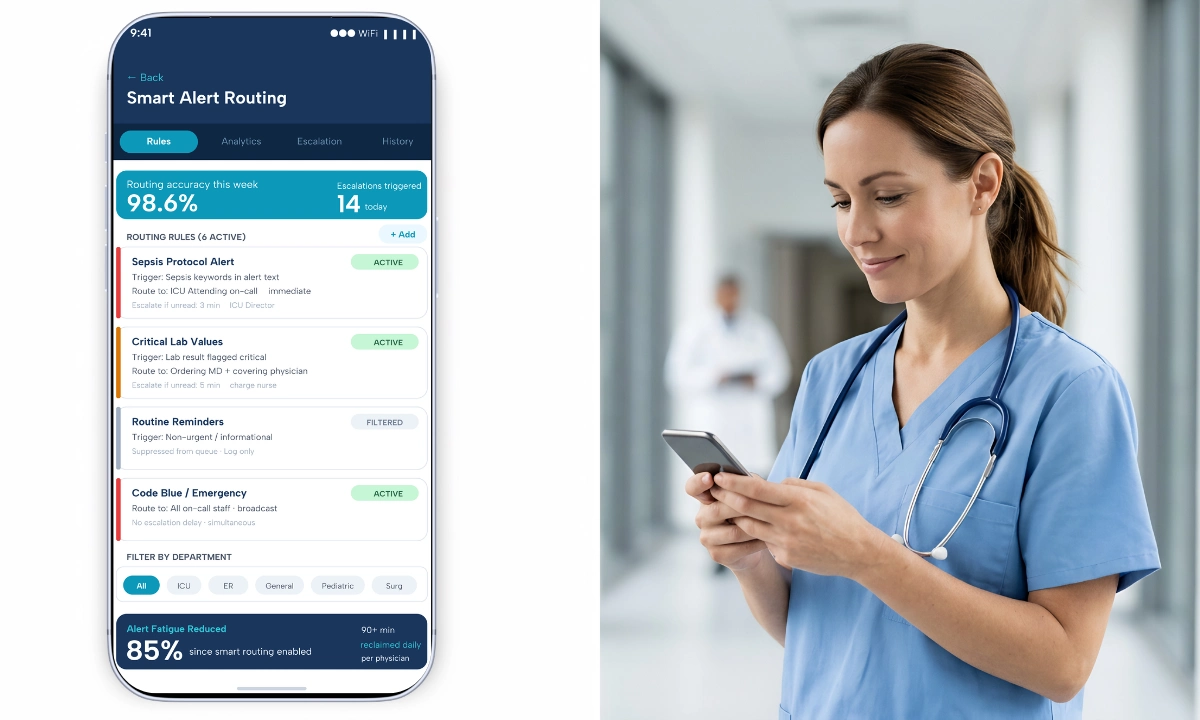
Modality Escalation Logic in Clinical Workflows
In high-acuity environments, communication modality is not arbitrary. Text may initiate a consultation, but voice clarifies urgency, and video confirms nuance.
A governed multi-modal communication system preserves this escalation pathway without losing context.
Fragmented tools force clinicians to restart conversations across channels, increasing cognitive switching costs and elevating error risk.
Unified Communication and Physician Burnout
The psychological toll of fragmented systems cannot be overstated. In a study highlighted that physician burnout rates reached 62.8%, with administrative barriers and chaotic work environments cited as leading contributors.
Many healthcare leaders now view communication infrastructure as a core physician burnout reduction strategy rather than a secondary IT investment.
To combat this, platforms must redefine the professional space. The D.O.C. (Doctor’s Opinion Count) Virtual Lounge serves as a private, physician-only space designed to recreate the traditional doctor’s lounge in a digital format. It is a HIPAA-compliant environment where verified physicians can unwind, share stories, and engage in specialty-specific forums. This space is critical for addressing the emotional exhaustion associated with burnout by fostering a sense of community among trusted peers. The Doctor’s Opinion Count Virtual Lounge is restricted to credentialed physicians to ensure a private and secure environment for peer-to-peer interaction, meaning administrative staff cannot access it.
Communication Governance as Clinical Infrastructure
Beyond the technical integration of tools, healthcare professionals require spaces that cater to their specific professional needs.
Effective governance requires distinct environments for different types of collaboration, a principle explored in greater depth within discussions on unified clinical communication architecture.
Purpose-built unified clinical communication ecosystems address this through distinct, governance-aligned environments:
- ClinicianCore HCO vs HCC: ClinicianCore HCO (HealthCare Organization) is designed for intra-office communication and focuses on unifying a single medical practice or department. In contrast, ClinicianCore HCC (HealthCare Collaboration) is designed for inter-organizational collaboration, allowing providers from different entities to consult and document cases together. ClinicianCore HCC uses a secure, AI-powered architecture that enables seamless communication across hospitals and clinics while maintaining strict encryption and identity-based security. This allows for inter-organizational connectivity without compromising patient privacy.
- HealthCare Xchange (HCX): In contrast to the clinical focus of other modules, HCX is intentionally not HIPAA compliant. The HealthCare Xchange (HCX) is designed for discussing high-level trends, innovations, and general medical data. This distinction is vital for fostering open conversations about healthcare trends, best practices, and innovation without the restrictions of protected health information (PHI) regulations. By remaining non-HIPAA compliant, ClinicianCore enables more flexible AI integration and open discussion, provided that no PHI is shared. A prominent banner always reminds users of this boundary. HCX leverages AI capabilities for trend analysis and expert matching, enabling visionaries to connect and collaborate on the future of medicine.
Unified Communication and Medical Practice Efficiency
The transition to a unified communication platform yields measurable improvements in both operational efficiency and provider satisfaction.
- Reduction in Documentation Time: Recent evidence published in JAMA Network Open (2025) examining ambient documentation technology across two academic medical centers found significant reductions in clinician burnout and improved documentation-related well-being. Clinicians using ambient documentation reported improved efficiency and reduced cognitive burden compared with baseline measures.
- Improved Retention: By reducing the friction of daily communication, organizations can mitigate the retention tax associated with clinician turnover. The cost of losing a single registered nurse averages approximately $61,110, according to the 2025 NSI National Health Care Retention Report.
- Enhanced Patient Safety: Unified inter-organizational collaboration platforms eliminate silos that contribute to medication errors and missed diagnoses during transitions of care.
- Revenue Cycle Optimization: In environments governed by CPT codes 99446–99452 for interprofessional consults, structured documentation is not optional, it is a reimbursement requirement. Through HealthCare Collaboration (HCC), the platform captures the clinical context, consult reasoning, and time attribution within the communication workflow itself. This embedded documentation trail strengthens audit readiness, preserves billing integrity, and ensures that physician coordination time is appropriately compensated.
Structured documentation pathways are especially critical for meeting strict interprofessional consult billing requirements in multi-specialty environments.
The Economic Case for Unified Communication Infrastructure
Communication inefficiency is not a workflow inconvenience, it is a balance sheet liability. When hospitals rely on siloed messaging systems, delayed consults, redundant documentation, and missed billing capture compound into measurable financial leakage.
An integrated clinical communication infrastructure consolidates workflows, reduces rework, and transforms previously unstructured consultative effort into documented, compliant activity.
Future-Proofing Healthcare Communication Infrastructure
Healthcare leaders investing in Multi-Modal Clinical Communication in Healthcare are not upgrading tools — they are redesigning communication architecture.
The integration of video, voice, and text through a purpose-built, physician-centric unified clinical communication platform is one of the most effective structural approaches to reducing burnout and improving care quality.
By providing clinicians with the tools to communicate naturally and the spaces to connect professionally, we can finally build a healthcare system that works for those who provide care as much as it works for those who receive it.
Fragmented Tools vs Integrated Clinical Communication Infrastructure
The contrast between fragmented systems and a unified clinical communication platform can be illustrated structurally:
| Feature / Metric | Fragmented Communication | Unified Clinical Communication Platform |
| Annual Cost of Inefficiency | Costs the US healthcare system $12 Billion annually. | Recaptures lost value by documenting consults for billable revenue. |
| Primary Channel Reliance | 86% of hospitals rely on email. | Integrates video, voice, and secure text. |
| Documentation Efficiency | Siloed and manual data entry. | Saves roughly 20% of documentation time via integrated tech. |
| Physician Burnout Impact | Contributes to a 62.8% burnout rate. | Fosters community and reduces administrative friction. |
| Information Delivery | Causes a “last-mile communication problem”. | Delivers asynchronous and real-time data seamlessly. |
Why Clinical Communication Infrastructure Is an Executive-Level Decision
Clinical communication architecture is no longer a frontline workflow preference. It is an enterprise governance decision that affects throughput, workforce stability, compliance exposure, and financial performance.
When video, voice, and text systems operate independently, leaders inherit hidden operational drag: prolonged length of stay, revenue leakage from undocumented consults, escalating burnout-related turnover costs, and fragmented audit trails.
Executive evaluation must shift from “tool selection” to infrastructure strategy.
Frequently Asked Questions
How does a unified clinical communication platform ensure data security across organizations?
A unified clinical communication platform ensures data security by embedding encryption, identity-based access controls, audit logging, and HIPAA-aligned governance directly into communication workflows. Rather than relying on disconnected tools, secure infrastructure centralizes video, voice, and text within a controlled environment designed to protect Protected Health Information (PHI).
– End-to-end encryption across modalities
– Role-based access and identity verification
– Audit trails for compliance monitoring
What is the difference between intra-office and inter-organizational communication modules?
Intra-office communication modules unify collaboration within a single medical practice or department. Inter-organizational modules extend secure communication across hospitals, specialists, and external providers, preserving documentation integrity while enabling structured consult workflows.
– Intra-office: Department-level workflow coordination
– Inter-organizational: Cross-entity consult collaboration
– Both operate under governance-aligned frameworks
Why would a healthcare communication environment intentionally not be HIPAA-compliant?
Some healthcare collaboration environments are intentionally non-HIPAA compliant because they are designed for general professional discussion, industry innovation, and trend analysis, not patient-specific information. These environments operate with clear boundaries prohibiting the exchange of PHI.
– Used for education, strategy, and innovation
– PHI sharing is explicitly restricted
– Clear governance notices maintain compliance boundaries
How does unified clinical communication support revenue cycle integrity?
A unified clinical communication platform supports revenue cycle integrity by embedding consult documentation, time attribution, and clinical reasoning directly within communication workflows. In environments governed by CPT codes 99446–99452, structured documentation strengthens audit readiness and reimbursement accuracy.
– Context captured at the point of care
– Reduced billing ambiguity
– Improved compliance alignment
Can administrative staff access secure physician-only collaboration spaces?
Physician-only collaboration environments are restricted to credentialed clinicians to preserve professional confidentiality and peer-level discussion. Administrative access is intentionally limited to maintain trust, psychological safety, and governance clarity within secure professional spaces.
– Access controlled by credential verification
– Separate from operational communication channels
– Designed to support professional peer exchange