The delivery of patient care relies on the rapid exchange of critical information. However, when clinical teams rely on fragmented tools to share Protected Health Information (PHI), they expose their organizations to severe regulatory risks.
Fragmented networks and consumer-grade apps create operational bottlenecks, delay patient care, and increase the likelihood of data breaches. Implementing robust HIPAA compliant communication in healthcare is no longer just a legal requirement; it is a foundational operational strategy that protects data while enabling seamless collaboration across the medical ecosystem.
More importantly, this level of compliance should not be treated as a standalone safeguard. It must function as infrastructure, embedded within a unified clinical communication framework that supports secure collaboration, intelligent routing, and operational efficiency across healthcare organizations.
Overview
HIPAA compliant communication in healthcare requires more than basic encryption. It demands secure clinical messaging systems built with end-to-end encryption, strict access controls, comprehensive audit logging, and signed Business Associate Agreements (BAAs). Healthcare organizations that implement secure healthcare communication platforms reduce compliance risk, eliminate shadow IT exposure, and improve medical practice efficiency. When embedded within a unified clinical communication infrastructure, HIPAA compliant collaboration becomes a strategic operational advantage rather than a regulatory obligation.
Key Takeaways
| Compliance Requirement | Operational Impact | Compliance Risk | Strategic Solution |
|---|---|---|---|
| Encryption of PHI | Secure transmission of patient data | Data breaches and regulatory penalties | Encrypted clinical messaging platform |
| Access controls | Controlled visibility of patient records | Unauthorized PHI exposure | Role-based secure collaboration |
| Audit logs | Traceable communication records | Legal vulnerability during audits | Centralized documentation system |
| Business Associate Agreements (BAAs) | Vendor accountability and governance | Institutional liability | Unified clinical communication infrastructure |
| Secure voice and messaging | Faster care coordination | Shadow IT usage | HIPAA compliant clinical communication software |
| AI-powered routing | Reduced alert fatigue and faster response times | Missed critical alerts | Intelligent smart routing engine |
What Does HIPAA Compliant Communication in Healthcare Really Mean?
HIPAA compliant communication in healthcare refers to secure clinical messaging systems designed to protect Protected Health Information (PHI) in accordance with the HIPAA Privacy Rule through strict access controls, audit logging, end-to-end encryption in healthcare environments, and legally binding Business Associate Agreements (BAAs).
It is a common misconception that simply using a password protected app ensures compliance. True HIPAA compliant communication in healthcare requires a comprehensive architecture designed specifically for medical workflows.
- PHI handling requirements: Every message, image, and lab result must be treated as secure data, protected both in transit and at rest.
- Encryption standards: Advanced cryptographic protocols must safeguard patient data from unauthorized interception.
- Access controls: Strict identity verification and role based permissions ensure only authorized personnel view specific patient records.
- Audit logs: Organizations must maintain immutable records tracking exactly who accessed or shared PHI, when, and from what device.
- Business Associate Agreements (BAAs): Vendors providing the communication infrastructure must sign legally binding agreements accepting responsibility for protecting patient data.
Why Traditional Messaging Fails HIPAA Compliant Communication in Healthcare
Clinical teams often bypass clunky Electronic Health Record (EHR) portals in favor of speed, inadvertently creating massive security vulnerabilities.
- Consumer apps: Standard messaging platforms lack the encryption and access controls required by federal law.
- Shadow IT: When doctors and nurses adopt unapproved software workarounds, IT departments lose visibility over where patient data resides.
- Lack of auditability: Consumer platforms cannot produce the detailed access logs required during a regulatory audit.
- No centralized governance: Without administrative oversight, organizations cannot remotely wipe data from lost or stolen devices, leading to catastrophic breaches.
The Hidden Operational Cost of Non-Compliant Communication in Healthcare
Operating outside of secure channels carries a steep price tag beyond regulatory fines.
- Revenue leakage: Informal curbside consults conducted via standard text messages are rarely documented in the EHR, leading to missed billing opportunities.
- Legal exposure: Data breaches result in massive federal penalties, class action lawsuits, and devastating damage to institutional reputation.
- Workflow inefficiencies: Searching for fragmented patient context across disparate apps drains clinical hours and delays critical interventions.
- Physician burnout: The cognitive burden of managing unorganized, unsecure communication channels exacerbates stress and pushes providers away from bedside care.
Core Components of HIPAA Compliant Clinical Communication Software
True HIPAA compliant clinical communication software must balance regulatory safeguards with clinical usability to ensure adoption across healthcare teams.
Modern platforms must bridge the gap between security and usability to ensure high adoption rates among medical staff.
- End-to-End Encryption in Healthcare: Securing data from the sender’s device all the way to the recipient’s screen to ensure PHI remains protected in transit and at rest.
- Role based access: Dynamically routing messages to the active on call specialist rather than a static directory name.
- Case based documentation: Grouping conversations by patient and episode of care to maintain clear clinical context.
- Secure voice and video: Enabling telehealth consultations and urgent verbal handoffs within the protected ecosystem.
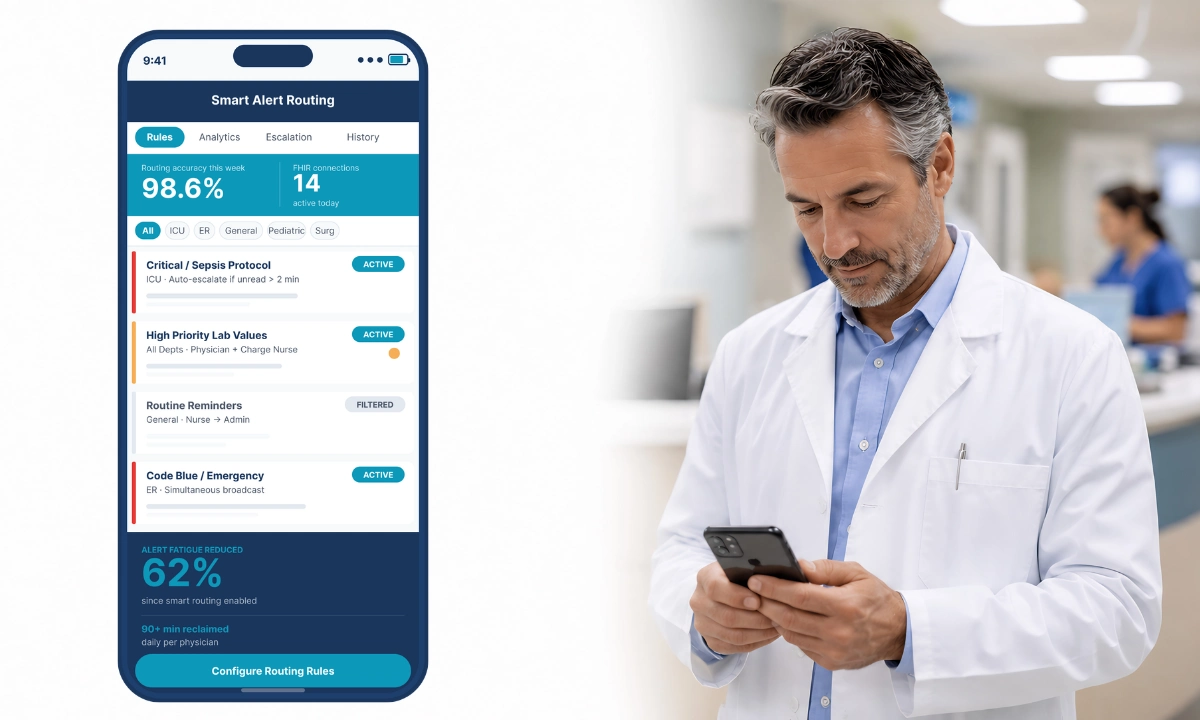
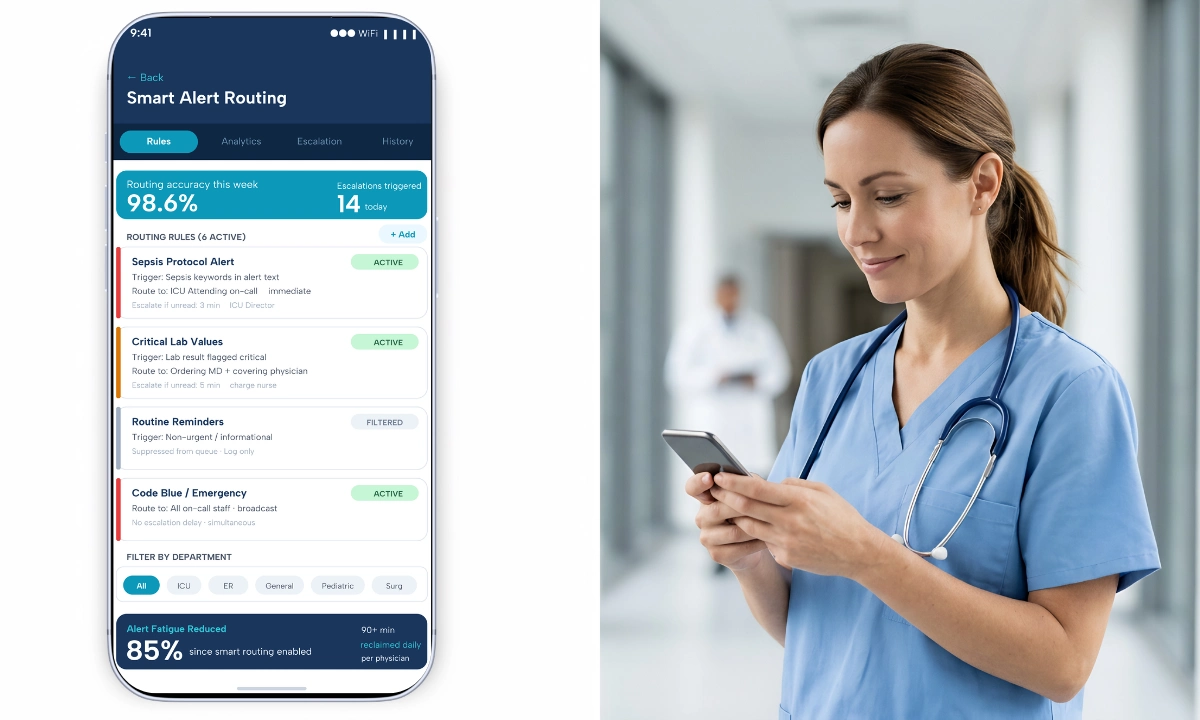
- AI powered smart routing: Utilizing advanced algorithms to filter non urgent alerts and direct critical information to the right provider instantly. This aligns with broader advancements in healthcare AI and innovation.
How HIPAA Compliant Collaboration Improves Medical Practice Efficiency
Secure communication is a powerful driver of operational ROI. When care teams utilize a unified platform, the time spent tracking down colleagues or waiting for callbacks drops significantly. This accelerated collaboration directly improves patient throughput and reduces average length of stay.
By integrating secure messaging with the EHR, physicians reclaim hours previously lost to administrative data entry.
This streamlined environment directly supports physician burnout reduction by minimizing alert fatigue, eliminating communication chaos, and restoring clarity across clinical workflows.
Organizations that invest in secure infrastructure consistently see measurable improvements in medical practice efficiency.
Conclusion
HIPAA compliant communication in healthcare is no longer optional. It is foundational infrastructure that protects patient data, enables secure collaboration, and directly supports medical practice efficiency.
Healthcare organizations that treat communication as a strategic infrastructure layer, not simply an IT add-on, are better positioned to reduce compliance risk, eliminate shadow IT, and restore clarity across clinical workflows.
A unified, physician-designed clinical communication platform provides the secure ecosystem necessary to sustain both regulatory compliance and operational excellence.
When implemented strategically, HIPAA compliant communication in healthcare becomes more than a regulatory requirement. It becomes enterprise infrastructure that supports unified clinical communication, healthcare AI-driven smart routing, and sustainable operational efficiency.
Frequently Asked Questions
What makes an app HIPAA compliant?
An app is HIPAA compliant if it encrypts Protected Health Information (PHI), enforces strict access controls, maintains comprehensive audit logs, and operates under a signed Business Associate Agreement (BAA).
Why is standard texting not HIPAA compliant in healthcare?
Standard SMS messages are not encrypted, lack centralized governance, and cannot provide audit trails, making them vulnerable to unauthorized PHI exposure.
How does secure messaging reduce physician burnout?
By consolidating fragmented tools into a unified platform, secure messaging reduces alert fatigue, speeds up consults, and minimizes administrative friction.
What is the role of AI in HIPAA compliant communication in healthcare?
Healthcare AI improves communication workflows by intelligently prioritizing urgent alerts, routing messages to the correct on-call staff, and reducing unnecessary interruptions.
Can HIPAA compliant platforms integrate with EHR systems?
Yes. Enterprise-grade clinical communication platforms integrate directly with EHR systems to centralize patient context and documentation within a secure ecosystem.